Process: Analysis of time taken to clerk patients in an A/E, Medical and GP Assessment Units during the 1st Quarter of 2019
The problem
The systems and processes in place within the Emergency Department, Medical Assessment Unit and the GP Assessment Unit were contributing to an extended length of time for clerking acute medical patients.
What we did
- 2 medical on call SHO’s were observed on 2 separate occasions for a total of 5.65 hours
- A timed record of activities/tasks was annotated breaking these tasks into patient specific tasks, non-specific patient tasks and interruptions
- A report which included waterfall charts of the timed activities with recommendations was presented to consultants and senior leadership within the organisation
What we achieved
We were able to identify several areas that, if implemented, would improve the patient experience, improve the timeliness of the processes and would utilise staffing resources in a more effective manner.
These included:
- Adoption of single, integrated clerking documentation
- Protocols developed and implemented for standardised tests to be requested and ordered at triage by nursing staff
- Use of physician assistants (or similar) for tasks that can be completed by a healthcare professional other than a doctor and implemented consistently across the 3 areas e.g. taking bloods, contacting residential homes to gain full history of reason why patient is presenting if not available
- Standardisation of paperwork, use of equipment and storage in ED, MAU & GP assessment unit
- The need for standardised protocols for common presentations to minimise variation, improve safety and flow e.g. dehydration
- Development of criteria to enable patients to be transferred to ward prior to Post-take consultation in simple cases to minimise time, if possible, in ED and to assist in development of management plan
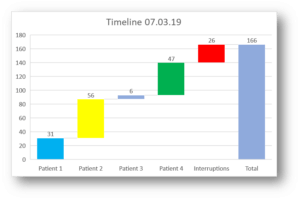
Analysis was provided on the amount of time spent clerking patients to support review of the process and highlight areas for further review or improvement:

This showed the variation in time to clerk patients but also highlighted how much time was lost due to interruptions. The detail behind the analysis was used to support formulation of actions to address both the variation and the process: